
Smarter Revenue Cycle Management for Modern Healthcare
Reduce claim rejections and accelerate reimbursements with structured and intelligent billing workflows built for today's providers.
Complete Revenue Cycle Solutions
End-to-end billing workflows designed to reduce denials, accelerate payments, and keep your practice financially healthy.
Front-End Optimization
Accurate patient data from day one
Demographic Entry
- Patient ID verification
- Insurance card data capture
- Address and contact validation
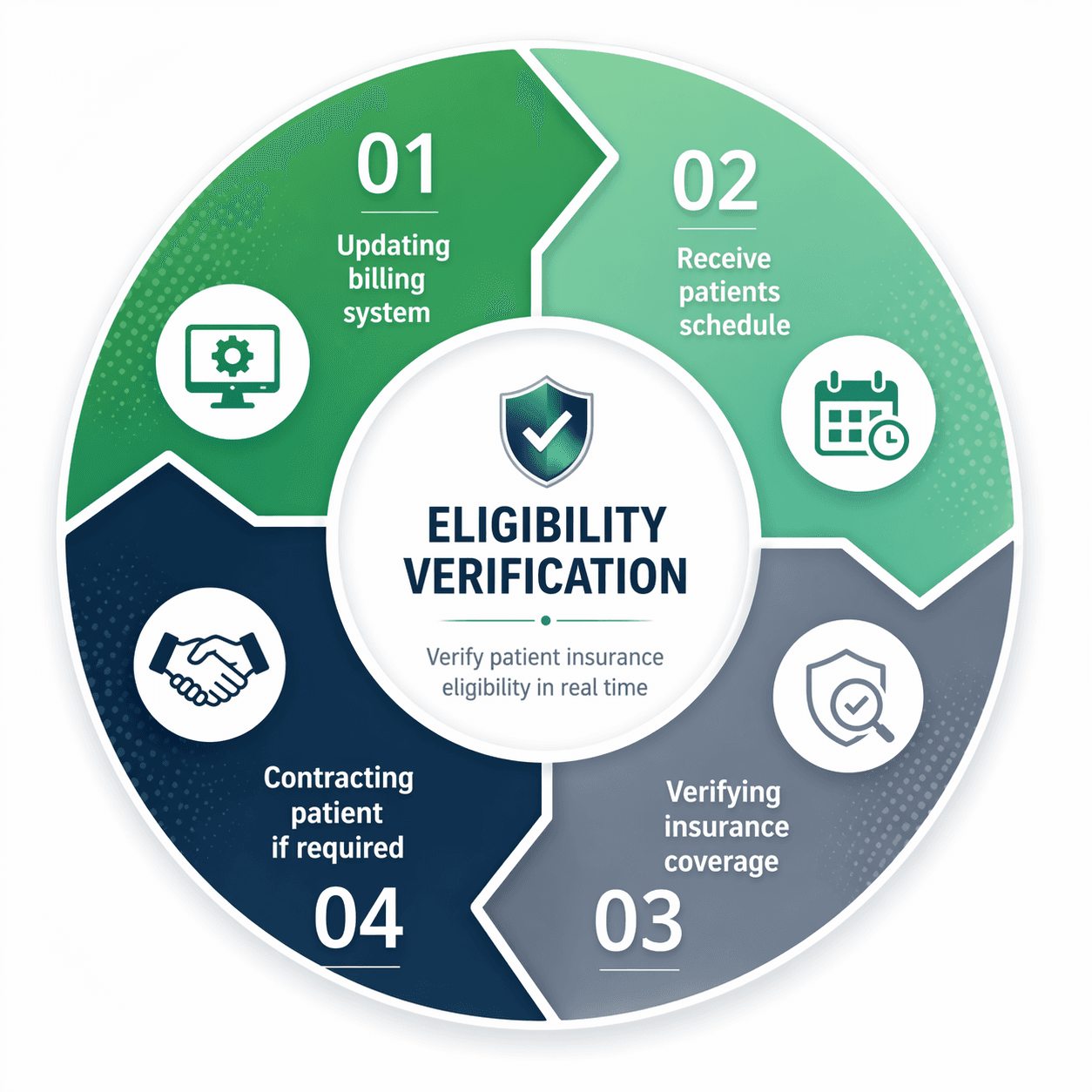
Eligibility Verification
- Real-time payer eligibility checks
- Benefits breakdown reporting
- Prior authorization tracking

Insurance Validation
- Network status verification
- COB identification
- Coverage gap alerts
Billing & Claims Processing
Clean claims submitted right the first time

Charge Entry
- CPT/ICD-10 code accuracy
- Modifier application
- Charge audit workflows

Claim Submission
- 837P/837I electronic claims
- Secondary claim follow-through
- Timely filing compliance

Clearinghouse Edits
- Edit identification & resolution
- Rejection trend analysis
- Same-day resubmission
Revenue Recovery
Recover every dollar you've earned

Payment Posting
- ERA/EOB payment posting
- Contractual adjustment application
- Patient balance reconciliation

Denial Management
- Denial categorization & tracking
- Level I & II appeal preparation
- Payer-specific appeal strategies

Credit Balance Review
- Overpayment identification
- Credit balance reporting
- Compliance documentation

Refund Processing
- CMS-compliant refund handling
- Refund letter preparation
- Audit trail maintenance
How We Optimize Your Revenue Cycle
A structured, prevention-first workflow that eliminates errors at every stage — from scheduling to final payment.
Appointment Scheduled
Patient appointment is booked and demographic data collection begins immediately.
Pre-Validation
Insurance eligibility verified, benefits confirmed, and prior authorizations obtained.
Charge Entry
CPT and ICD-10 codes entered with modifiers applied and charge audit completed.
Claim Submission
Clean 837P/837I electronic claims submitted to payers via clearinghouse.
Rejection Handling
Clearinghouse edits identified, resolved, and claims resubmitted same day.
Denial Management
Denied claims categorized, appealed with payer-specific strategies at Level I & II.
Payment Flow
ERA/EOB posting, patient balance billing, and A/R follow-up completed.
Prevention-First Philosophy
Our workflow is engineered to catch errors before they become denials. By front-loading eligibility verification, code accuracy, and authorization tracking, we reduce downstream rework and accelerate your cash flow from the very first touchpoint.
Built on a Foundation of Trust
Every engagement is backed by enterprise-grade security, regulatory compliance, and contractual safeguards.
HIPAA & PHI Safeguards
- ✓Full HIPAA Privacy & Security Rule compliance
- ✓PHI handled under strict access controls
- ✓Regular compliance audits and staff training
- ✓Breach notification protocols in place
Data Security Controls
- ✓AES-256 encryption at rest and in transit
- ✓Multi-factor authentication enforced
- ✓Secure VPN and network segmentation
- ✓Continuous monitoring and threat detection
Legal & Contractual Compliance
- ✓Business Associate Agreements (BAA) executed
- ✓NDA signed with all staff and contractors
- ✓CMS and payer-specific compliance adherence
- ✓Documented policies and procedures
Access & Identity Management
- ✓Role-based access control (RBAC) enforced
- ✓Least-privilege access principles applied
- ✓Audit logs for all data access events
- ✓Immediate access revocation on offboarding
Ready to sign a BAA?
We execute Business Associate Agreements before any data is shared.
A Purpose-Built Billing Partner
We combine deep revenue cycle expertise with modern technology to deliver measurable financial outcomes for healthcare providers of every size.
Provixion Technologies was founded with a singular focus: to give healthcare providers the financial clarity and operational efficiency they deserve. We combine deep RCM expertise with modern technology to deliver measurable results across every stage of the revenue cycle.
Our team of certified billing specialists, compliance officers, and technology professionals work as an extension of your practice — not just a vendor. We understand the nuances of payer behavior, coding requirements, and regulatory obligations that directly impact your bottom line.
From solo practitioners to multi-specialty groups, we tailor our workflows to fit your unique needs, ensuring every claim is submitted correctly, every denial is challenged, and every dollar is recovered.
Simplify revenue cycle management so providers can focus on patient care, not paperwork.
A healthcare ecosystem where billing complexity never stands between providers and their revenue.
Technology-Led
Automation and intelligent workflows reduce manual errors and speed up reimbursements.
People-First
Certified billing specialists who act as a true extension of your practice team.
Outcome-Driven
Every engagement is measured against clean claim rate, denial rate, and days in A/R.
Software Platforms We Support
Schedule a Consultation
Tell us about your practice and we'll show you exactly how we can improve your revenue cycle performance.
Flexible engagement models tailored to your practice size and billing volume. Start with a free revenue cycle assessment.